2018 FSA Posters
P019: ANESTHETIC MANAGEMENT OF PULMONARY ALVEOLAR PROTEINOSIS, A CASE REPORT
Samantha Ford, MD, Ross Renew, MD; Mayo Clinic
Introduction: Pulmonary alveolar proteinosis is a diffuse lung disease in which periodic acid Schiff positive lipoproteinaceous material accumulates in the alveoli. Primary congenital and secondary adult forms occur. Patients experience dyspnea, cough, decreased PaO2 and an increased A-a gradient. Treatment is targeted towards etiology and may include whole lung lavage. This requires special considerations for anesthetic management.
Background: Anesthesia for patients with pulmonary alveolar proteinosis poses unique challenges. Whole lung lavage is one of the few absolute indications for use of double lumen endotracheal tubes. Impediments to delivering a safe and effective anesthetic include management of physiologic derangements and technical aspects of the lavage itself.
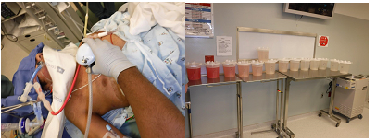
Case Presentation: A 30-year-old previously healthy male was transferred from an outside hospital with respiratory distress. He was initially diagnosed with pneumonia and treated with antibiotics and steroids. His respiratory function worsened and required high flow oxygen therapy. Lung biopsy revealed alveolar proteinosis. Whole lung lavage proceeded under general anesthesia in the operating room. Standard ASA monitors with a radial arterial line were used. General anesthesia was induced with propofol and rocuronium and maintained with sevoflurane. A left sided double lumen tube was placed. Positioned supine, the left lung was ventilated while the right lung was lavaged with warmed saline via a 3-way drainage system. External percussion was performed to facilitate mobilization of intra-alveolar debris.
Intraoperative complications included hypoxemia and hypotension. Other issues that arose were construction of infusion tubing, and facilitation of instillation drainage. Our equipment required an adaptor to securely fit the infusion tubing to our DLT. Repeated lateral tilt/ Trendelenburg positioning was necessary to facilitate passive fluid drainage. Our patient experienced repeated episodes of hypoxemia following drainage of each aliquot of instilled fluid. After repeat fiberoptic exam to confirm DLT position and rule out fluid cross over to the ventilated lung, V/Q mismatch was diagnosed. Our patient also experienced repeated hypotension with percussion of the chest wall. Vasopressor support was provided and frequent breaks in percussion were required to maintain adequate blood pressure. The patient received three whole lung lavages on sequential days; two of the right and one of the left lung. He was discharged after 4 days to a specialty hospital for inhaled GM-CSF therapy.
Discussion: Anesthetic management of PAP requiring whole lung lavage draws special considerations. Equipment setup prior must ensure seamless fluid transfer. Lung isolation with a double lumen endotracheal tube is required. A well thought out differential for complications will aid proper management. Patient positioning can be altered from supine to lateral decubitus to assist with V/Q matching. Extracorporeal membranous oxygenation may be necessary for some patients with severely compromised gas exchange. Fastidious measurement of instilled and drained fluid along with monitoring of oxygenation and airway pressures is necessary to guarantee no fluid is retained inside the lungs. PAP patients can experience significant improvement in their symptoms with possible sustained remission after WLL. Anesthesia providers play an important role in the success of the procedure.