2018 FSA Posters
P007: A LOW COST TASK TRAINER FOR FRONT-OF-NECK EMERGENCY AIRWAY ACCESS TRAINING
Samsun Lampotang, PhD, Cameron R Smith, MD, Anthony Destephens, Lauren Berkow, MD, Nikolaus Gravenstein, MD, Felipe Urdaneta, MD, PhD; University of Florida
Introduction: Front-of-neck techniques to secure a difficult airway in a cannot intubate - cannot oxygenate scenario are the final common pathway in the ASA difficult airway algorithm. Since emergent cricothryotomies are not commonly performed procedures, anesthesiologists are often hesitant to use them and unfamiliar with the equipment necessary or available at their institution. Previous studies have shown that simulation can be highly efficacious to familiarize anesthesiologists with the tools and techniques at their disposal during airway emergencies. Unfortunately, purpose-built simulators for front-of-neck airway access training are scarce, expensive to obtain, and require the ongoing purchase of relatively high-cost consumables for continued use. Likewise, there is a scarcity and high cost associated with the use of cadavers for such training and practice. By modifying the design originally proposed by Varaday et al (2004), we have implemented a low cost, easy to produce and sufficiently realistic simulation task trainer to help fill this gap and describe its use.
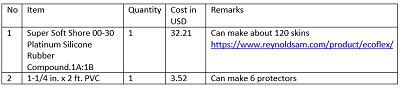
Assembly: Using readily available hospital supplies that are very inexpensively acquired, a standard intubation simulator (e.g., Laerdal) can be quickly and easily modified to also be used for front-of-neck airway access training without compromising its utility as an intubation trainer. We begin with a section of corrugated tubing sourced from a ventilator circuit. Into this tubing, we place heavy paper cut from a file folder to simulate the posterior tracheal membrane, which is free of cartilaginous rings. We place behind the tubing a 4” section of 1-1/4” diameter PVC pipe cut longitudinally to protect the intubation mannequin from inadvertent damage from overzealous needle placement. Over the corrugated tubing, a layer of silicone compound made from Ecoflex 00-30 Platinum Silicone Rubber Compound is placed to simulate skin and soft tissue. Once assembled this unit can be secured to the exterior of an intubation training mannequin using self-adhesive dressing, e.g., Coban®. The simulator is now ready for use.
Results: To date, this simulator has been used during difficult airway exercises at the University of Florida Center for Simulation, Safety & Advanced Learning Technologies with over 200 anesthesiologists to practice multiple techniques for front-of-neck emergency airway access. This task trainer lends itself well to practice the Difficult Airway Society’s new preferred front of neck access using a tube exchanger vs. a Seldinger-style technique. Response to the trainer has been universally positive across the entire experience spectrum, from medical students through experienced anesthesiologists.
Conclusions: We believe that the task trainer we describe is easy and inexpensive to make. Additionally, deliberate practice of front-of-neck emergency airway access techniques provided by the task trainer helped to increase familiarity and confidence with performing such techniques, as illustrated by unsolicited feedback from a trainee informing us 2 weeks post-training that our training helped provide a good outcome in an actual difficult airway requiring cricothyrotomy.